Reopening Guide
As you consider expanding your patient services understand that is it each provider’s responsibility to determine how their practice will operate. PCS has prepared an extensive guide for consideration (below) but understand that not all guidelines apply to every practice.
However, regardless of practice size or location, there are certain essential elements to consider. Click the link below for our essentials list:
REOPENING CHECKLIST

Before reopening you should have a plan and establish appropriate protocols within your office. You can use the list below and the associated hyperlinked sections as a checklist and guide. Note: some of these actions are not required but most are recommended when they apply to your individual practice.
- Communicate with and care for staff
- Train staff on job-specific PPE and COVID guidelines
- Prepare the office
- Establish/review appropriate protocols on sterilizing all equipment
- Prepare patient care areas
- Establish appropriate protocols on sterilizing frames
- Inventory existing supplies and estimate needs to maintain recommended PPE
- Review CDC hand hygiene guidelines
- Outline workload plans for staff and identify strategies to manage patient flow
- Establish triage protocols
- Develop screening protocols for staff and patients
- Develop patient interaction protocols
- Communicate with patients
- Resources
COMMUNICATE WITH AND CARE FOR STAFF

Communicate
- Stay in contact with staff during this time. Consider utilizing a communications tree or webinars.
- Communication is very important; staff would rather hear you tell them that you don’t have the answers than to not hear from you until you do.
- Demonstrate consideration for the mental health of the staff and team while reestablishing the new care delivery flow.
Ensure a positive work environment
- INVOLVE your staff in decision making – they often know office operations better than you do.
- Eliminate or reduce tasks that are not contributing to improved patient care.
- Facilitate access to support programs, if possible.
- Encourage balance.
Educate
Educate Staff About
- Coronavirus disease 2019 (COVID-19).
- Importance of containing the outbreak.
- Facility policies and practices to minimize the chance of exposure.
- Job-or task-specific information on preventing transmission of infectious agents.
- How to advise patients about changes in office procedures (e.g., calling prior to arrival if the patient has any signs of a respiratory infection and taking appropriate preventive actions).
- Family management plans if they are exposed to COVID-19.
TRAIN STAFF

Train staff should on job-specific PPE and demonstrate competency with selection and proper use of PPE.
Standard Precautions
- Hand hygiene with soap and water or use of hand sanitizer.
- Use of personal protective equipment (masks, gloves, etc) as needed.
- Respiratory hygiene/cough etiquette as spelled out by the CDC.
- Clean and disinfected environmental surfaces.
Optometrists will meet with all staff and present the COVID-19 guidelines and instructions.
- Strict adherence to hand hygiene including:
- before and after contact with patients;
- after contact with contaminated surfaces or equipment; and
- after removing PPE.
- Daily Staff Health Screening: Take staff temperature before workday begins.
- If below 100.4 degrees, employee may work.
- If above 100.4 degrees, employee sent home or referred to a testing center based on answers to the COVID-19 questionnaire.
PREPARE THE OFFICE

General Considerations
- Place barriers to cover high touch frequency items when possible.
- Remove all items that cannot be disinfected from the waiting area and the patient care areas such as:
- magazines,
- other paper materials,
- remote controls,
- toys, etc.
- Maintain proper air circulation (use only HEPA filtration)
- Consider
- disinfectant foggers (use with caution).
- UV devices.
- barriers and shields.
- Limit / eliminate cash.
- Move credit card processor to patient only touch.
- Think about everything that is touched – pens, coffee service, etc.
Post signage
- Post signage at the entrance and inside the office to alert all patients with respiratory symptoms and fever to notify staff immediately.
- Post signage with pictures to teach/remind all patients about correct respiratory hygiene and cough etiquette. Specifically, they should cough and sneeze into a tissue (which then should be properly discarded), or into the upper sleeve.
- Remind patients to use appropriate handwashing techniques.
Cleaning
Clean and sanitize/wipe down with EPA approved disinfectants:
- Countertops after each patient encounter
- Phones, including receiver and touchpad
- Keyboards – all office computers
- Doors, especially where someone would grab to open or shut
- Doorknobs, drawer pulls, cabinet knobs
- Pens (for patient use, keep a clearly marked supply of sanitized and non-sanitized pens)
- Dispensing mats
- Light switches
- Water cooler handles
- Coffee machine buttons
- Chair arms, in waiting area and back offices
- Tables
- Clip boards
- Computer mice
- Laptop exteriors
- Keys and key rings
- Faucets
- Flush handles
- Optical tool handles
- On/off switches for all devices in the front office
Provide Supplies For Patients
- Provide no-touch waste containers with disposable liners in all reception, waiting, patient care, and restroom areas.
- Provide alcohol-based hand rub and masks in all reception, waiting, patient care, and restroom areas.
- Always keep soap dispensers stocked and consider handwashing signs in those areas.
CLEAN EQUIPMENT

Guidelines for equipment used in patient care
- Use disposable equipment when possible. Single use equipment should not be reused unless cleaning and disinfection procedures are provided by the manufacturer.
- Protect reusable equipment from gross contamination with blood and body fluids as much as possible.
- Reusable equipment that has been in direct contact with the patient should be cleaned and reprocessed before reuse.
- Consider protective gloves when cleaning soiled equipment or other soiled areas.
- Procedures should be established for assigning responsibility and accountability for routine cleaning of all patient care equipment.
PREPARE PATIENT CARE AREAS
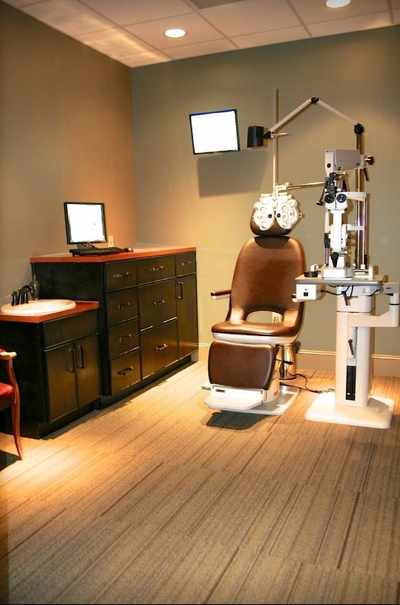
These items/areas are important for patient safety and should be cleaned thoroughly
- Pretest equipment (including the outsides of the machines where patients touch)
- Pretest tables
- Occluders (paddles)
- Projector knobs / Remotes
- Laminated / reusable sheets
- Slit lamps
- Refractors
- Trial contact lens displays / Trial lens scanner
- Trial frames and lenses
- Exam chairs
- Stools
- Hard surface seats
- Color / stereo test books
- Pupilometers
- Lensometers
- PD rulers
- Office supplies (staplers, dispensers, etc.)
- The outside of handheld condensing lenses
- Limit Goldmann tonometry
ESTABLISH FRAME CLEANING PROTOCOL

All frames should be cleaned after any patient has tried them on
- All frames should be rubbed down on the temples, eye wires, bridge and nose pads.
- Considerations for cleaning frames include:
- Hot, soapy water
- Ultrasonic cleaners
- UV sanitizers
- Non-toxic disinfectants (like hydrogen peroxide)
- Avoid cleaning frames with alcohol or any disinfectant product that could damage the frame material.
INVENTORY PPE

General Notes
Considering that patients who are asymptomatic may still be COVID-19 infectious, it should be assumed that all patients can transmit disease. Optometrists must exercise their independent professional judgment and carefully consider the availability of appropriate PPE to minimize risk of virus transmission.
Personal Protective Equipment
- Face-masks Note: Surgical masks are best – N95 not necessary per CDC unless you are treating a patient with active or suspected COVID infection.
- Gloves.
- Eye protection.
- Access to germicidal wipes.
- Ample supply of hand sanitizer.
- Soap and water.
Face mask notes
- Rotate reusable masks every four days Note: Do not attempt to clean an N95 mask.
- Anything is better than nothing – hand made masks are OK if you cannot obtain medical masks.
- Best material for hand made mask is standard cotton.
- Make sure covers mouth, nose and fits under chin.
- Wash nightly – HOT water.
- Can clean with hydrogen peroxide.
Evaluate supply chain
Identify materials and supplies required for care to be delivered during an outbreak or pandemic, and suppliers that can provide those materials. Order appropriate materials and supplies.
Clothing
- All staff (including doctor) should wear machine washable clothing.
- Lab coats, if worn should be cleaned nightly in hot water.
- Consider wiping down shoes when returning home and leaving them outside to prevent spread.
REVIEW CDC HAND HYGIENE

Routine Patient Care
Use an Alcohol-Based Hand Sanitizer
- Immediately before touching a patient.
- Before performing an aseptic task (e.g., placing an indwelling device) or handling invasive medical devices.
- After touching a patient or the patient’s immediate environment.
- After contact with blood, bodily fluids, or contaminated surfaces.
- Immediately after glove removal.
Wash with Soap and Water
- When hands are visibly soiled.
- After caring for a person with known or suspected infectious diarrhea.
- After known or suspected exposure to spores (e.g. B. anthracis, C difficile outbreaks).
Notes
- Alcohol-based hand sanitizers are the most effective products for reducing the number of germs on the hands of healthcare providers.
- Alcohol-based hand sanitizers are the preferred method for cleaning your hands in most clinical situations.
- Wash your hands with soap and water whenever they are visibly dirty, before eating, and after using the restroom.
Guidelines for Hand Hygiene in Healthcare Settings
- When cleaning your hands with soap and water, wet your hands first with water, apply the amount of product recommended by the manufacturer to your hands, and rub your hands together vigorously for at least 15 seconds, covering all surfaces of the hands and fingers.
- Rinse your hands with water and use disposable towels to dry. Use the towel to turn off the faucet.
- Avoid using hot water to prevent drying of skin.
Gloves
- Wear gloves, according to Standard Precautions, when it can be reasonably anticipated that contact with blood or other potentially infectious materials, mucous membranes, non-intact skin, potentially contaminated skin or contaminated equipment could occur.
- Gloves are not a substitute for hand hygiene.
- Never wear the same pair of gloves in the care of more than one patient.
- Carefully remove gloves to prevent hand contamination.
- You can use sanitizers and wash your gloves without removing them.
ESTABLISH WORKLOAD PROTOCOLS
Outline Workload Plans For Staff
Prepare staff for cleaning and sanitizing, while safely keeping up with patient flow as best as possible.
Opening Cleaning Protocol
Follow the protocol described above for cleaning:
Closing Cleaning Protocol
Follow the protocol described above for cleaning:
Equipment and Exam Room Cleaning Protocol in Between Patients
- After delivering care, exit the room as quickly and directly as possible.
- Complete documentation in clean area.
- Clean room and all medical equipment completely with appropriate cleaning solutions.
ESTABLISH WORKFLOW PROTOCOLS
Manage patient flow
Identify strategies for your office that manage patient flow and ensure appropriate physical distancing, including, but not limited to:
- Re-evaluate office flow and waiting area capacity.
- Re-arrange reception / seating area to maintain social distancing.
- Request patients call or text the office upon arrival.
- Instruct patients that companions should remain outside of the facility and not accompany the patient into the facility unless they are a parent/guardian of the patient or if they are a true caregiver and need to assist the patient.
- Establish a longer time frame in between patient appointment.
- Consider limiting the number of patient visits per day.
Automate check in
- Phone interview prior to appointment.
- Online history.
- Tablet for history and patient forms.
Customize frame selection and dispensing
- Re-arrange optical dispensary.
- Optician MUST be more in charge.
- Bring frames to the patient.
Provide Barriers
- Slit lamp breath shield.
- Refractor breath shields.
- Consider sneeze barriers.
ESTABLISH TRIAGE PROTOCOLS

Decide the order to schedule patients
- Prioritize those patients that require urgent or emergent care.
- Patients with complex cases that need follow up.
- Patients with expired prescriptions.
- Next confirm any appointments already on the schedule after open date.
- Next schedule those with original appointments that were cancelled.
- Accept new appointments.
DEVELOP SCREENING PROTOCOLS FOR STAFF AND PATIENTS
Screen everyone
- Screen patients, visitors and staff members for symptoms of COVID-19 prior to and/or upon their arrival at the facility, including utilizing non-contact temperature readers. (Questionnaire provided below).
- Any staff member showing signs of being sick or any temperature above 100 degrees should not be permitted to work and should be referred to their primary care provider.
- Patients and visitors exhibiting signs of being sick or any temperature above 100 degrees should be rescheduled, unless an emergency dictates otherwise, and referred to their primary care provider.
COVID-19 Questionnaire
- Do you have any of the following symptoms? Fever, sore throat, cough, shortness of breath?
- Have you recently lost your sense of smell or taste?
- Do you have any GI symptoms? Diarrhea? Nausea?
- Even if you don’t currently have any of the above symptoms, have you experienced any of these symptoms in the last 14 days?
- Have you been in contact with someone who has tested positive in the last 14 days?
- Have you traveled outside the United States by air or cruise ship in the past 14 days?
- Have you traveled within the United States by air, bus or train within the past 14 days?
Optometric Personnel Considerations
- If HCP is sick, tests positive for COVID-19, or is caring for an individual that tested positive for COVID-19, the HCP should not report to work.
- Pregnancy: There is limited data currently available regarding susceptibility of COVID-19 and the severity of infection in pregnant women. Pregnant staff are encouraged to consult with their health care provider. Pregnant staff are encouraged to clean hands often using soap and water or alcohol-based hand sanitizer and clean and disinfect frequently touched surfaces.
Notes
- If possible, schedule appointments apart enough to minimize possible contact with other patients in the waiting room.
- Remind patients to limit the number of companions.
- Depending on office size, patients may need to wait in their vehicles or outside until their appointment.
- Companions may need to wait in their personal vehicles or outside.
- Trace instructions: Instruct patient to contact office if they experience COVID-19 symptoms within 14 days after their eye exam.
DEVELOP PATIENT INTERACTION PROTOCOLS

Upon Arrival
- Check temperature.
- Confirm COVID-19 questionnaire before proceeding with exam.
Provide patients with instructions
- Keep 6 feet from all other individuals when possible.
- Proper hand hygiene.
- Proper respiratory hygiene and cough etiquette.
Utilize Barriers
If possible, have a clear barrier separating front desk staff from patients. Otherwise, try to maintain distance when possible between front desk and patients when conducting office functions such as accepting payments, scheduling future appointments, etc.
- Depending on office size, patients may need to wait in their personal vehicles or outside the optometric office until their appointment.
- Companions may need to wait in their personal vehicles or outside the office.
- If possible, separate patients by 6 feet in the waiting area or have barriers separating patients in the waiting area.
Remove items
Remove all items that cannot be disinfected from the waiting area and the patient care areas such as:
- Magazines.
- Other paper materials.
- Remote controls.
- Toys, etc.
- Place barriers to cover high touch items when possible.
Notes
- HCP should adhere to Standard Precautions.
- Disinfect high-frequency touch surfaces often.
- Provide hand sanitizer throughout the optometric office.
* Treating patients at higher-risk: COVID-19 is a new disease and there is limited information regarding risk factors for severe illness. Consider separate office hours for patients at higher-risk due to comorbidities or age.
COMMUNICATE WITH PATIENTS
Stay in contact through all relevant communications channels
- Website, social media, email, direct mail, advertising.
- Update your website, social media channels and phone voicemail to communicate that your office is open for eye health and vision care and use the opportunity to reinforce the importance for the care you deliver and how you are taking steps to protect patient and staff health and safety.
- Utilized automated technologies when possible.
- Remind your patients, when relevant, that you are open for essential routine and urgent care, emergencies, telehealth consultations, questions and concerns.
- Ensure that all communications reinforce your practice safety protocols.
Utilize Telehealth
When appropriate for patients, CMS and CDC strongly encourage utilizing telehealth to prioritize inpatient care for those who have urgent needs. You can:
- Read our telehealth summary.
- Read our article in ROB.
- View our webinar or telehealth (50 minutes).
Notify Patients
Based on expectations for a return to routine care, begin booking routine appointments for an anticipated day one re-activation and beyond (be sure to make patients aware there remains a chance the limited schedule order may not be lifted).
Contact and check-up on your complex patients
- Diabetic retinopathy.
- Glaucoma.
- Age-related macular degeneration.
- Complex contact lens patients (e.g., scleral).
- Myopia management patients.
- Refractive surgery referrals.
- Patients that refer.
Identify patients whose care has been postponed
- Individuals referred for non-urgent surgery and/or routine care.
- Alert those who may need to reschedule or restart their authorization and scheduling process.
RESOURCES

The following resources are helpful:
- CDC Hand Hygiene in Healthcare Settings
- CDC: Strategies for Optimizing the Supply of Isolation Gowns
- CDC: Strategies to Optimize the Supply of PPE and Equipment
- CDC: Steps Healthcare Facilities Can Take Now to Prepare for COVID-19
- CDC: Characteristics of Health Care Personnel with COVID-19
- OSHA: Guidance on Preparing Workplaces for COVID-19
- AOA: Optometry practice reactivation preparedness guide
- CMS: Re-opening Facilities to Provide Non-emergent Non-COVID-19 Healthcare: Phase I
- COVID Exposure Risk Assessment & Recommended Guidelines
COMPLETE REOPENING GUIDE (PDF)


